The 2026 IME Market Report
By Chloe Smith | May. 13, 2026 | 10 min. read
Executive Summary
We surveyed claims professionals across the United States to understand how Independent Medical Examinations (IMEs) – evaluations conducted by a neutral, third-party physician – are being used today, what drives their use, and what this reveals about the gap between where the market currently is and where it needs to be.
Three key findings define the current landscape:
The market is stable but carrying more weight per claim.
70% of respondents report no change in IME volume, yet medical severity rose by 6% in 2024 alone and remains elevated according to the latest NCCI updates. Fewer claims are reaching the IME stage, and the ones that do carry higher financial exposure.
IMEs are being used to resolve medical uncertainty, and expectations need to reflect that.
When asked what drives the decision to order an IME, 42% of respondents cited clarifying causation and resolving conflicting opinions. When asked to identify the single most valuable outcome, 44% pointed to a clear determination of causation. When the goal is a defensible medical decision, quality becomes the priority, and higher-quality IMEs require more time and higher cost. That reality makes timing and expectation setting important early in the claim.
There’s a quality gap.
More than 1 in 3 respondents rated their IME vendor a 3 out of 5 or lower. Less than 1 in 5 gave a top score. Slow turnaround, scheduling delays, and reports that lack clarity are the most common frustrations. These issues point to a broader concern around consistency and report quality: vendors optimizing volume over rigor.
These key findings suggest that IME usage may be stable, but its role has become more concentrated. Claims that progress to an IME today are more complex and carry greater financial and legal impact, which raises the importance of reaching a clear and defensible conclusion. The survey data indicates the vendor market has not fully adapted to that reality, with performance patterns that continue to favor volume over the level of analysis these claims demand.
Section 1: A Stable Market Carrying Higher Stakes
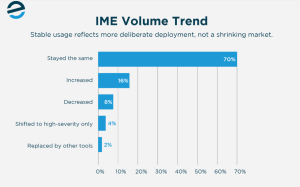
IME usage has held steady, with 70% of respondents reporting no change in volume over the past 12 months. That stability takes on a different meaning when viewed against broader claim trends.
Claim frequency declined 5% in accident year 2024, the third consecutive year of above-average declines, while medical severity increased by 6%, with recent updates indicating that pressure on claims costs is continuing. For high-cost claims exceeding $5 million, medical expenses account for approximately 90% of total costs.
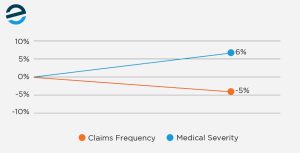
Early-intervention protocols and medical-cost-containment regulations have also reduced escalation in simpler cases. This includes faster claim reporting, earlier contact with injured workers, increased use of nurse case management, and tighter controls around treatment authorization and provider selection. These steps resolve many routine issues before they develop into larger disputes. As a result, more straightforward claims are resolved earlier and do not progress to the IME stage.
With fewer claims overall, stable IME volume suggests that examinations are being used consistently, but within a narrower portion of the claim population. A larger share of IMEs is now tied to higher-severity claims with greater financial impact. This points to a shift toward more selective use, even if overall volume remains unchanged.
Section 2: Why IMEs Get Ordered – And What That Tells Us
When claims professionals order an IME, they are trying to resolve a medical narrative that is unclear, incomplete, or contested. That has not changed.
Causation and conflicting opinions account for 42% of all cited ordering reasons. This remains the primary driver, ahead of litigation defense, cost control, and severity combined. That priority carries through to outcomes – 44% of respondents say clear causation determination provides the most value from an IME.
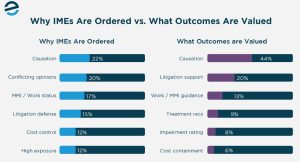
Medical opinions frequently diverge, and that divergence is often centered on causation and work-relatedness, which is exactly why IMEs exist.
The role of an IME has remained consistent: to answer a medical question that directly affects how the claim moves forward. What has changed is where the question is addressed. In many cases, it is no longer the first step.
Lower-complexity claims are increasingly resolved earlier through tools like peer review, utilization review, and nurse case management. By the time an IME is introduced, the file has often already been evaluated, and the remaining issue is more disputed or more consequential.
This creates a higher expectation for what a quality IME must deliver. A causation determination on a routine claim carries limited impact, while that same determination on a high-exposure claim can influence reserve decisions and litigation strategy.
Section 3: What Is Shifting IME Behavior
The market narrative often cites technology as the primary driver of change in the IME market – AI, analytics, telemedicine, and digital transformation. While these forces are at play, adjusters report that day-to-day shifts are more closely tied to workflow decisions.
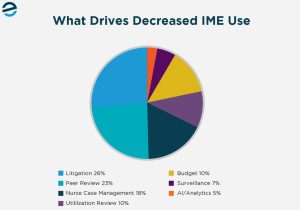
Among respondents who reported decreased IME usage, litigation strategy shifts (26%) and increased peer review (23%) were the top picks. AI and analytics tools accounted for just 5% of responses. The changes happening in practice are driven by how a claim is being litigated and whether a paper-based review or nurse case management is sufficient before escalating to a full examination.
In many cases, peer review is used to determine whether a formal exam is necessary, helping control costs and avoid over-deploying IMEs on straightforward claims. At the same time, litigation strategy is shaping when IMEs are ordered, with exams more often reserved for cases where the opinion will directly impact defense, settlement, or trial outcomes.
So, the question becomes: when is a peer review enough, and when does a claim require an IME?

Peer Review vs. IME: Knowing When Each Tool Belongs
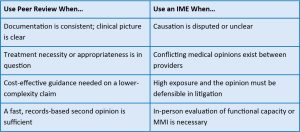
Peer review and IMEs serve different functions, and conflating them creates risk. Peer review is a records-based assessment, often used when the medical record is complete and internally consistent. It provides a faster opinion at a lower cost in lower-complexity claims, where a full examination may not add meaningful value.
An IME requires a physical evaluation by an independent physician and produces an opinion grounded in direct clinical observation. It becomes necessary when the file does not resolve the core issue, especially in cases involving disputed causation or conflicting medical opinions. Because it involves scheduling, exam time, and a detailed report, it takes longer and costs more than peer review, but that added time and expense are what allow the physician to assess credibility and apply clinical judgment in a way the record alone cannot.
Survey findings suggest increased reliance on peer review as an initial clinical filter. This aligns with broader workers’ compensation trends toward utilization review, nurse case management, and file-based physician assessment before pursuing the more costly, time-intensive IMEs. However, peer review is unlikely to replace IMEs in complex or disputed cases; rather, it is more often used to determine whether an IME is truly necessary.

Section 4: The Quality Gap – Where the Market Falls Short
Satisfaction with IME vendors is far from strong — 1 in 3 respondents rated their vendor average or worse, while fewer than 20% gave a top score. That gap suggests IME providers are clearing the bar on basics, but falling short when it comes to the clarity and efficiency that claims really demand.

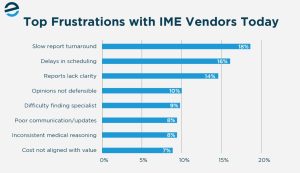
The top complaints are operational: slow report turnaround (18%), scheduling delays (16%), and reports that lack clarity (14%). Opinions not defensible in litigation (10%) and difficulty finding the right specialist (9%) follow closely behind.
Scheduling constraints are, in part, a structural problem. The AAMC projects a shortage of up to 86,000 physicians by 2036, with surgical specialties among the most affected. These specialties are among the most in-demand for IMEs and the most difficult to schedule. Physician availability directly limits what any vendor can deliver in terms of timeline.
But the complaints about clarity and defensibility signal something far more fundamental.
The Deeper Problem: Volume Over Rigor
IME vendors operating at scale often prioritize speed and geographic coverage. This means larger physician panels, standardized workflows, and faster report turnaround targets, which improve efficiency but can limit the depth of analysis in more complex cases.
The result is reports that are completed quickly but rely on generalized language or incomplete clinical integration. When a report does not fully address the referral question, it creates another decision point. That can mean follow-up reviews, supplemental questions, or a second IME before anything can move forward.
Research supports what adjusters are experiencing firsthand – IME quality is not consistently applied across examinations, with documented gaps in patient-centered analysis and integration of clinical information. The AMA Guides and ACOEM set a clear standard: medical opinions grounded in evidence-based medicine and reasoned, case-specific analysis. But in high-volume environments, maintaining that level of rigor becomes more difficult.
This creates a tradeoff across the market. Vendors focused on speed and cost tend to deliver faster turnaround times. Vendors focused on quality tend to require more time and higher cost. The difference shows up in whether the IME resolves the issue or extends the claim.
Section 5: What A Good IME Vendor Looks Like
The characteristics that distinguish vendors who consistently clear that bar are not complicated, but they require intentional investment that volume-first business models may not prioritize.
Physician Vetting: More Than a License Check
Good physician vetting means confirming the physician is actively practicing, holds the right specialty for the claim at hand, and has no history of sanctions or exclusions. It’s also important to consider the physician’s practice mix. Courts may scrutinize opinions from physicians who perform a high volume of insurance work, so vendors with rigorous, balanced vetting protocols help ensure that reports are well supported and more likely to withstand challenge.
Report Quality Assurance: The Question That Has to Get Answered
A quality assurance process should check whether the physician addressed the specific referral questions, whether the reasoning is grounded in the clinical findings, and whether the conclusions would survive cross-examination. A report that restates the medical record without drawing a defensible conclusion hasn’t done the job, regardless of how quickly it arrived.
Specialty Depth, Not Just Panel Size
A large physician network is only useful if the right specialist is available for your specific claim. When causation is disputed or the injury is complex, a vendor’s ability to match you with the right examiner, not just the nearest one, makes a major difference in opinion quality.
Proactive Communication as a Standard
Much of the friction behind the top complaints in our survey stems from simply not knowing where a claim stands. A vendor that keeps you informed at each step saves your team significant time and reduces the back-and-forth that compounds delays.

Section 6: What Claims Professionals Should Do Now
1. Match the tool to the question
IMEs are most effective when the claim outcome depends on resolving a clinical question with high exposure attached. In cases where documentation is consistent and the clinical picture is clear, peer review or utilization review may be the right first step. But deploying the wrong tool for the situation only creates more problems downstream.
Using an IME in a low-complexity situation adds time and cost without improving the outcome. Using peer review in a complex situation can delay resolution and create additional steps later. The goal is to avoid introducing a second decision point.
2. Be deliberate about timing
Timing directly impacts whether an IME provides value. If the clinical picture is still evolving, the report may not provide a clear answer. If the IME is ordered too late, the claim carries unresolved exposure longer than necessary. The trigger for ordering should be a considered decision based on where the claim stands, not a default response to stagnation or an arbitrary stage in the claim lifecycle.
Ordering earlier in the decision-making process increases the likelihood of a usable outcome, especially when it is clear that causation or conflicting opinions will not resolve on their own.
Timelines should also reflect the type of examiner required. Specialists are more difficult to schedule and often require longer lead times. Higher-quality IMEs, particularly those involving the right specialist, take longer and cost more. Setting realistic expectations early helps avoid delays later in the claim.
3. Evaluate your vendor relationships with the same rigor you’d apply to the claim
The survey data suggests many claims professionals are working with results that do not fully meet expectations. Vendor performance should be measured by whether the IME resolves the question the first time.
Faster, lower-cost exams may appear efficient, but if they lead to additional reviews or repeat IMEs, total claim duration and cost increase. Actively evaluating vendor performance – and being willing to act on what you find – yields outcomes more likely to justify the investment.
Sources
American Medical Association. (2025, December 4). AMA Guides® to the Evaluation of Permanent Impairment: an overview. AMA. https://www.ama-assn.org/practice-management/ama-guides/ama-guides-evaluation-permanent-impairment-overview
Association of American Medical Colleges. (2024, March). The Complexities of Physician Supply and Demand: Projections From 2021 to 2036. AAMC. https://www.aamc.org/media/75231/download
Currey, J., & Sprogis, S. K. (2024, October 24). Conceptualising the quality experience for independent medical examinations: A narrative review. ScienceDirect. https://www.med.upenn.edu/pmi/events/https-www-sciencedirect-com-science-article-abs-pii-s1047847720300046-via-3dihub
National Council on Compensation Insurance. (2024). 2024 Regulatory and Legislative Trends Report. NCCI. https://www.ncci.com/Articles/Documents/II_Regulatory-Legislative-Trends2024.pdf
National Council on Compensation Insurance. (2025, May 13). 2025 State of the Line Guide. NCCI. https://www.ncci.com/SecureDocuments/SOLGuide_2025.html
Pitfalls during times that compromise IME reports. Weber Legal Nurse Consulting Inc. (2024, December 31). https://www.weberlegalnurse.com/pitfalls-during-times-that-compromise-ime-reports
Rohom, K. (2026, April). Independent Medical Evaluation Service Market Size 2026-2032. 360iResearch. https://www.360iresearch.com/library/intelligence/independent-medical-evaluation-service
